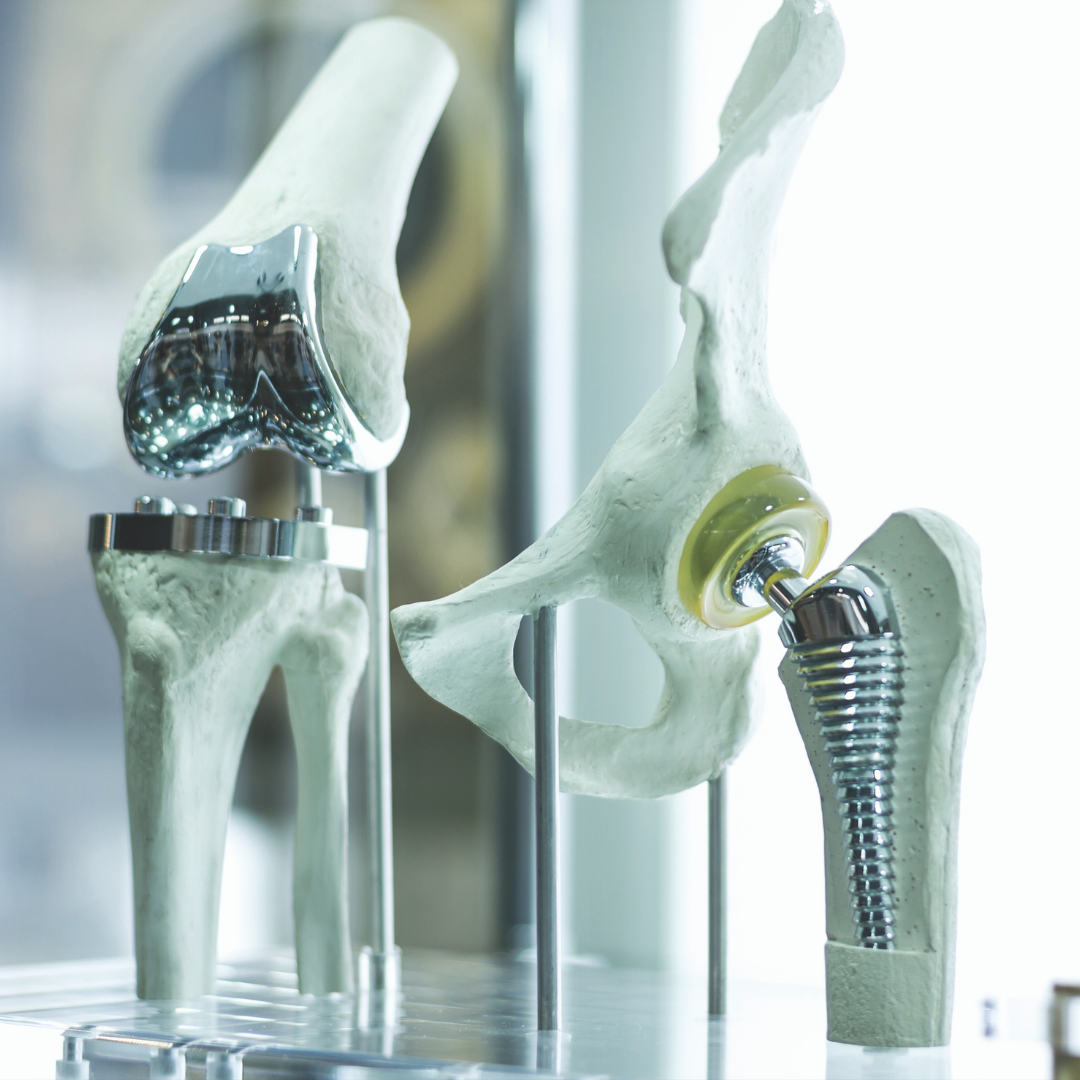
Total joint replacement procedures such as total knee and total hip arthroplasty are among some of the most successful operations that we have in orthopedic surgery. Often, the operations provide significant pain relief for patients who have debilitating arthritis and severe symptoms. Surprisingly, both procedures have changed very little over the past 30 years. The total knee and total hip replacement components and techniques we use are very similar to the original techniques that were described in the 1970s. However, numerous advances have occurred over the years. Occasionally, it has been two steps forward and one step back, as some of the so-called advancements that were developed proved not to be beneficial over time. However, in general, substantial improvements have occurred. These advances could be categorized as advancements in technique, orthopedic materials, and anesthesia.
Total Joint Replacement Techniques
Minimally Invasive Surgery
One of the exciting advancements in total joint replacement surgery that has received considerable media attention in the last 5 years is the advent of minimally invasive surgery. Minimally invasive total hip replacement surgery was developed several years ago by Dr. Richard Berger in Chicago. The surgery involved the use of smaller incisions to insert the hip replacement components. This resulted in less pain after surgery, less blood loss, and a faster recovery. Soon after, minimally invasive total knee replacement surgery was pioneered with the concept that involves smaller incisions, less muscle dissection, and faster recovery as with the total hip replacement. When the techniques were initially developed, they were met with enthusiasm both by orthopedic surgeons and by the patients.
In the early days of the minimally invasive technique certain pitfalls and problems that could be associated with the procedure were not appreciated, which resulted in increased complications. Since that time, we have come to realize the limitations and which patients are the best candidates for the surgery. It has been shown that minimally invasive surgery is less invasive than traditional surgery, particularly for the skin incision. However, it has also been shown that the benefits of the procedure are not as dramatic as was initially felt.
However, one thing is for certain. The “minimally invasive movement” has made surgeons realize that our incisions can be smaller and our anesthesia techniques better, so as to decrease, but not eliminate, postoperative pain and speeding recovery. Not all patients are good candidates for less invasive surgery. Patients who are significantly overweight, who have had prior surgery, or who have substantial osteoporosis, or weakening of the bones, are not appropriate candidates for the procedure.
Computer Navigation
Another exciting advancement in total joint replacement surgery involves the use of computers during the operation. Though we have not yet advanced to the point of “robotic surgery”, surgeons are beginning to use computers to assist them in the operating room.
Slight malalignment of the limb after surgery can occur and can lead to premature wearing of the hip or knee replacement parts; this can lead to the need for further surgery. A computer is used in the operating room as a tool to help surgeons to perform their operation more precisely. While performing the surgery, the surgeon looks at the video monitor where he or she sees a display of the hip or the knee while the surgical procedure is carried out.
There are some disadvantages to the use of computer navigation in the operating room; however, the disadvantages are far outweighed by the benefits of improved alignment of the limb. The risks must be weighed against the potential benefit of improved limb alignment.
Materials for Total Joint Replacement
Bearing Surface
The original total hip replacement and total knee replacement involved the use of metal and plastic parts. The typical joint replacement would involve smooth metal bearings that are shaped either like the end of the thighbone in the case of a knee, or like the top of the thighbone in the case of the hip. These parts rub against a hard plastic liner. This creates a hard smooth surface for movement of the joint. We still use the original plastic material today that was used in the late 1960s and early 1970s for many procedures. However, refinements in the material have been made through the years, including the use of x-ray beams to improve the strength and life expectancy of the plastic. This material is called “highly cross-linked polyethylene.”
In addition, newer materials have been developed to use instead of the classic steel ball and plastic socket, including ceramic materials for the hip and the use of a metal socket instead of a plastic socket (“metal-on-metal hip replacement”). It is thought that the newer materials will prolong the lifespan of the joint replacement and put off the need for further surgery on the joint.
Bone Ingrowth Surfaces
Many types of joint replacements rely on the patient’s bone to grow into tiny pores in the prosthesis. This process is called “ingrowth”. It takes several weeks for bone ingrowth to occur. Once it does, the implants are firmly anchored to the prosthesis, hopefully forever. However, some patients have a bone that is damaged or of poor quality. This is often found in patients who are undergoing operations on their hip or knee for the second or third time. In these patients, the typical metal used for bone ingrowth may not always work.
New materials have been developed to improve the chances of bone ingrowth. One such material, called ‘trabecular metal”, is a metal that has a honeycomb pattern if looked at under a microscope. This stimulates bone to grow into the tiny honeycomb webbing. Research has shown that bone grows into this metal at a much faster rate than traditional metal surfaces. This has greatly improved our ability to repeat hip and knee surgery and with much better results.
Anesthesia
Finally, improvements in our anesthesia techniques have significantly improved the overall patient experience. For post-operation patients, the pain after surgery in the hospital is one of the most unpleasant aspects of the procedure. In the past, patients were put to sleep; after surgery, they would experience significant pain that would have to be controlled with pain medication. While this is still done in a significant number of cases, some patients are candidates for “regional anesthesia.”
An example of regional anesthesia is a spinal, where a needle is injected into the back to numb the legs from the waist down. This has been done for many years, but is currently being done more to improve pain after surgery even in patients who go do sleep. Additionally, a “nerve block” can be used. A nerve block involves injecting numbing medicine around one of the large nerves in the leg to “numb” the joint. This also decreases the pain that the patient experiences after surgery.
Newer oral medications are also in use to help control pain after the surgery, including “Cox-2 inhibitors” such as the anti-inflammatory drug Celebrex. These medications decrease pain by decreasing inflammation around the joint.
What’s next for Total Joint Replacement
Hip and knee replacement surgery remain as some of the best operations that we have in orthopedic surgery. They are very successful and patients have a high satisfaction rate in the vast majority of cases. However, we are always looking for ways to improve our results. We hope the advancements in total joint replacement surgery will continue. Further work and research will continue to improve our results and make the procedures even better for future patients.
James E. McGrory, MD
Columbus, Georgia
Last edited on April 10, 2024